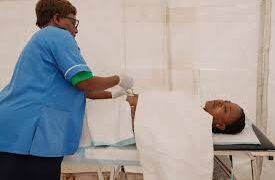
Dozens of young women, mothers carrying babies and men gathered in a dusty on the outskirts of Harare on Thursday to receive injections of a new HIV prevention drug, lenacapavir, recently introduced in Zimbabwe.
The country, which has recorded tens of thousands of HIV-related deaths over the past two decades, is among the first to roll out the twice-yearly injectable medication. Lenacapavir requires only two doses per year and has shown near-total protection against HIV infection in clinical trials.
Health officials have described the drug as a potential turning point in HIV prevention, particularly for high-risk groups. However, experts caution that funding shortages, weak health infrastructure and patient follow-up challenges could limit its broader impact.
At the launch event, 27-year-old sex worker Constance Mukoloka expressed relief after receiving one of the first doses under the donor-supported rollout across 10 African countries.
“I am safe, I can work with confidence now,” she said.
Mukoloka explained that daily oral preventive pills often exposed her to stigma. “When I took tablets, customers would see a container of pills and leave. They couldn’t tell the difference between prevention and treatment drugs,” she said, noting that the misunderstanding affected her income.
Lenacapavir was developed by Gilead Sciences and is being introduced in selected countries with support from PEPFAR and the Global Fund. In Zimbabwe, the injection is being offered free of charge to high-risk populations, including sex workers, adolescent girls and young women, gay men, and pregnant and breastfeeding women.
While Zimbabwe has long provided access to daily oral pre-exposure prophylaxis (PrEP), condoms, vaginal rings and shorter-acting injectables, adherence has remained a challenge, especially for individuals dealing with stigma or irregular routines.
“I work in beer halls looking for clients. Sometimes I would get drunk and forget to take my drugs. Sometimes I would work all night and not have time to take tablets,” Mukoloka said.
Despite progress in reducing HIV prevalence, new infections remain a concern, particularly among adolescent girls and young women. According to UNAIDS, women and girls accounted for 63 per cent of new HIV infections in sub-Saharan Africa in 2024, driven by poverty, gender inequality and limited access to healthcare.
Zimbabwean authorities say about 46,000 people across 24 sites are expected to benefit from the first phase of the rollout in a country of roughly 15 million people. Officials hope to expand access as more donor-funded doses arrive and are exploring options to procure additional supplies independently, though funding constraints remain a hurdle.
Medical professionals have welcomed lenacapavir as a major advancement but stress that it should complement—not replace—existing prevention tools.
Dr Ernest Chikwati of the AIDS Healthcare Foundation in Zimbabwe described the injection as a “game-changer,” while cautioning that it is “not a silver bullet.” He emphasized the continued importance of affordable prevention measures such as condoms.
For early recipients like Mukoloka, however, the new injection already represents a significant shift—offering protection, privacy and renewed confidence.